Learn More About Platelet-Rich Plasma (PRP) Therapy
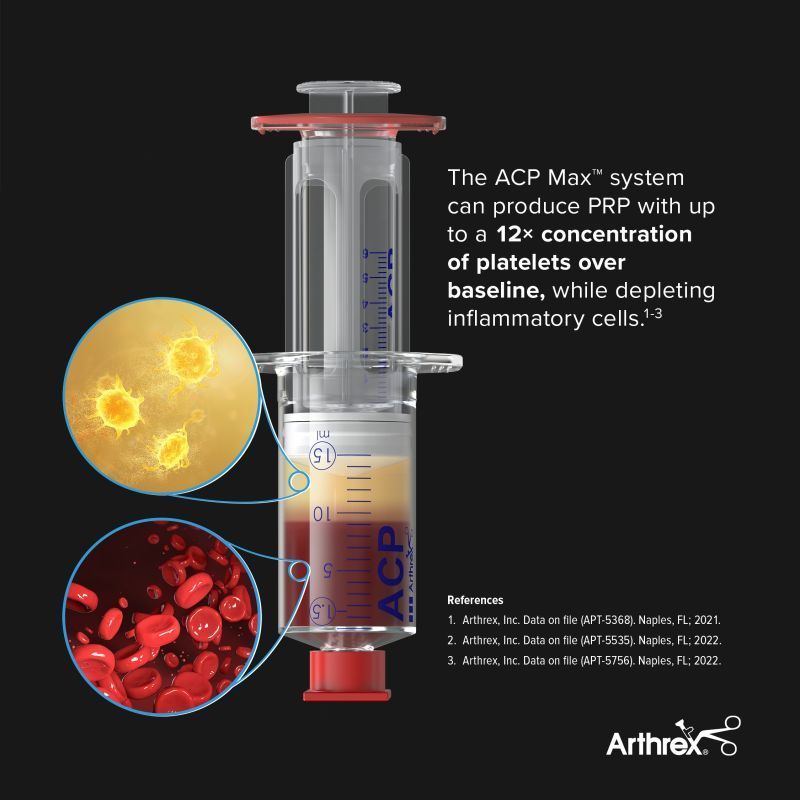
What Is PRP?
If you've been dealing with joint pain, tendon problems, or bursitis that hasn't fully responded to physical therapy or cortisone shots, your doctor may have mentioned platelet-rich plasma — commonly called PRP. It sounds technical, but the concept is straightforward: we take a small sample of your own blood, process it in a specialized centrifuge to concentrate the healing components, and inject that concentrate back into the area causing your pain.
The key ingredient in PRP is your platelets — tiny blood cells best known for helping wounds clot. What makes them valuable for treating joint and tendon problems is that they also carry a rich supply of proteins called growth factors. These growth factors act as signals that tell surrounding cells to reduce inflammation, recruit repair cells to the area, and help protect tissue from further breakdown.
The system we use — the Arthrex ACP Max — is a closed, sterile double-spin process that concentrates your platelets to roughly 10-12 times their normal level in the blood. This high-yield approach maximizes the amount of healing protein delivered to the target area in a single injection.
How Does It Work?
Once injected into a joint, tendon, or bursal space, the platelets become activated and release their growth factors into the local environment. Those growth factors then do several useful things:
Calm persistent inflammation. In arthritis and chronic tendon problems, the body gets stuck in a cycle of low-grade inflammation that slowly damages tissue. PRP helps interrupt that cycle by dialing down the inflammatory signals — without the side effects associated with repeated cortisone injections.
Protect remaining cartilage and tendon. PRP appears to slow the activity of enzymes that break down cartilage and tendon fibers, giving existing tissue a better chance of holding up over time.
Stimulate the body's own repair cells. Growth factors can recruit stem cells and other repair cells to the area, which may help maintain tissue health even if they don't rebuild significant new tissue.
The important thing to understand is that PRP works primarily by changing the environment in and around the joint — reducing harmful inflammation and slowing breakdown — rather than by regrowing lost cartilage or tendon from scratch. More on that below.
Where Is PRP Used?
Knee Arthritis
Knee osteoarthritis is where PRP has its strongest track record. A large 2023 analysis combining results from 35 clinical trials and more than 3,100 patients found that PRP outperformed both cortisone and hyaluronic acid ("gel injections") for pain relief and improved function, particularly at 6 and 12 months (Qiao et al., 2023). Results are best for mild to moderate arthritis — the treatment becomes less effective when joint damage is very advanced.
Another comprehensive review of 78 clinical trials involving over 5,000 patients found consistent pain reduction with PRP at 3 months that actually strengthened by the 12-month mark — the opposite of what happens with cortisone, which tends to wear off over time (Moraes et al., PubMed).
Hip Arthritis
The evidence for hip arthritis is promising but less consistent than for the knee. A 2023 meta-analysis found that PRP provided significantly better pain and function scores than gel injections at 6 months (Scoping Review, PMC). Results at 12 months are more variable across studies. Overall, PRP for hip arthritis appears most useful when other conservative options haven't provided adequate relief.
Shoulder: Rotator Cuff and Bursitis
For rotator cuff tendinopathy and shoulder bursitis, PRP and cortisone each have their role. Cortisone works faster and is often the better choice for an acute flare. PRP, on the other hand, tends to provide more durable relief — studies show that while cortisone patients may feel better sooner, PRP patients catch up and often surpass them at the 3-month mark and beyond, with greater improvements in pain and shoulder motion (PMC Orthopedic Review). For patients with ongoing tendon problems who have already had cortisone shots, PRP offers a meaningful alternative with a different mechanism of action.
What Are the Chances It Will Help?
No treatment works for everyone, and PRP is no exception. Based on the published research and clinical experience, roughly 60–70% of well-selected patients achieve meaningful improvement in pain and function that lasts 6 months or more. That's a reasonable success rate for a condition that otherwise has limited non-surgical options.
You're more likely to respond well if you have mild to moderate arthritis (rather than bone-on-bone), a healthy body weight, and no underlying inflammatory arthritis like rheumatoid arthritis.
One Shot or Several?
How many injections are needed is one of the most common questions patients ask — and the research gives a nuanced answer. A systematic review comparing single versus multiple PRP injections found that a single injection was equally effective for pain relief as multiple injections, though multiple injections showed a modest advantage for joint function at 6 months (Sánchez et al., PubMed). A more recent review concluded that three injections may outperform one for pain relief over the course of a year (Tao et al., Arthroscopy 2023), and a well-designed 2-year clinical trial found that multiple doses extended the benefit, though both single and multiple-dose patients ended up at similar levels by the 2-year mark (Yurtbay et al., PubMed 2022).
Our approach is to start with a single injection and see how you respond over the following 4–8 weeks. This makes practical sense: it identifies whether you're a good responder before committing to additional injections, and many patients get substantial relief from just one. If you respond well, a follow-up injection several months later can reinforce and extend that benefit.
Will PRP Rebuild My Cartilage or Tendons?
This is probably the most important question to address honestly, because it's easy to come across marketing that overpromises on this point. The short answer is: current evidence does not support meaningful cartilage or tendon regeneration from PRP injections.
Lab studies show that PRP growth factors can stimulate cartilage and tendon cells to produce more repair proteins — which is encouraging. But when researchers have used MRI scans to look for actual changes in cartilage thickness before and after PRP treatment in real patients, the results are generally not significant. One careful study using serial MRI found no meaningful change in cartilage thickness despite real improvements in pain and function (PMC Prospective Study). A systematic review of all available MRI evidence concluded that PRP should not be used with the expectation of growing new cartilage (da Ponte et al., ScienceDirect 2022).
What PRP appears to do well is slow the progression of damage and reduce the inflammation driving your symptoms — which translates into real, meaningful pain relief and better function for many patients. That's a worthwhile goal even without structural regeneration. Think of it less like rebuilding a worn-out part and more like giving the joint a better environment to maintain itself.
Is PRP Safe?
Because PRP is made from your own blood, the risk of allergic reaction or rejection is extremely low. The most common side effect is temporary soreness and swelling at the injection site for a few days after the procedure, which is a normal part of the inflammatory response triggered by the platelets activating. Serious complications are rare. Studies consistently report a favorable safety profile with no significant adverse events at standard dosing.
One thing to keep in mind: PRP is not a quick fix. Unlike a cortisone shot, which can reduce inflammation within days, PRP works more gradually. In our experience, most patients begin to notice meaningful pain relief around 2–3 weeks after the injection, with continued improvement over the following weeks as the growth factors do their work. It is important to give the treatment time before drawing conclusions about whether it is helping.
The Bottom Line
PRP is a well-studied, biologically sound treatment for arthritis, tendon conditions, and bursitis of the hip, knee, and shoulder. It works by delivering a concentrated dose of your body's own healing proteins to reduce inflammation and protect tissue — not by regrowing lost cartilage or tendon. About 2 out of 3 patients with appropriate conditions see meaningful improvement that lasts 6 months or more. A single injection is a reasonable first step; additional injections can extend the benefit for those who respond. If you have mild to moderate arthritis or a tendon problem that hasn't fully resolved with other treatments, it's worth a conversation about whether PRP makes sense for your situation.
References
- Qiao et al. (2023) — Network meta-analysis of 35 RCTs, 3,100+ patients, Knee OA (via PMC)
- Moraes et al. — 78 RCTs, 5,308 patients, PRP for orthopedic pain (PubMed)
- Scoping Review — PRP for Knee and Hip OA (PMC, 2024)
- PMC Orthopedic Review — PRP for Shoulder, Rotator Cuff (2023)
- Sánchez et al. (2019) — Single vs. multiple PRP injections, systematic review (PubMed)
- Tao et al. (2023) — 3 doses vs. 1 dose PRP in knee OA (Arthroscopy)
- Yurtbay et al. (2022) — Multiple vs. single PRP, 2-year RCT (PubMed)
- da Ponte et al. (2022) — PRP and cartilage regeneration on MRI, systematic review (ScienceDirect)
- PMC Prospective Study — MRI cartilage changes after PRP, 6-month follow-up
More Recent Articles